Osteoarthritis (OA) of the shoulder is a progressive joint condition that results from the breakdown of cartilage, causing pain, stiffness, and reduced function. Although less common than hip or knee OA, it can have a significant impact on quality of life—especially when it affects sleep, work, or daily activities. OA can affect either the glenohumeral joint (the ball-and-socket part of the shoulder) or the acromioclavicular (AC) joint, located at the top of the shoulder.
As joint surfaces wear down, the smooth cartilage lining the bones becomes thin and rough, leading to inflammation, pain, and eventual joint stiffness. While there is no cure for OA, many patients experience excellent symptom control with a combination of physiotherapy, activity modification, medication, and, when necessary, surgical intervention.

Anatomy of the Shoulder
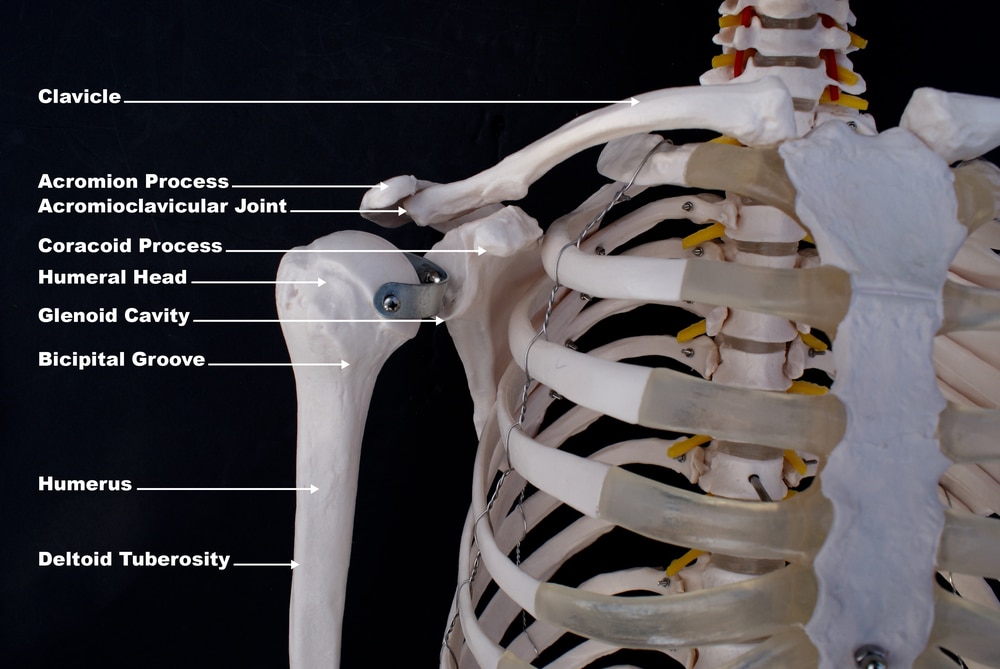
The shoulder is a complex joint system comprising:
● The glenohumeral joint, formed between the humeral head (ball) and the glenoid (socket) of the scapula
● The acromioclavicular joint, between the acromion (part of the shoulder blade) and the clavicle (collarbone)
Both joints are lined with articular cartilage, which allows smooth, pain-free motion. Surrounding the joints are ligaments, tendons, muscles (including the rotator cuff), and a lubricating joint capsule. With osteoarthritis, this cartilage breaks down, bone surfaces become exposed, and the body may form osteophytes (bone spurs) that further restrict movement.
Causes of Shoulder Osteoarthritis
Shoulder OA develops due to a combination of age-related degeneration, joint wear and tear, and in some cases, previous injury or surgery.
It can be classified as:
Primary OA
This occurs as part of the natural ageing process. Cartilage deteriorates over time, particularly in individuals over 60. It is more common in people who have led physically demanding lives or performed years of repetitive shoulder use.
Secondary OA
This results from:
- Previous trauma (e.g., fracture or dislocation)
- Chronic rotator cuff tears (leading to cuff tear arthropathy)
- Inflammatory conditions such as rheumatoid arthritis
- Avascular necrosis, where reduced blood supply leads to joint surface collapse
- Previous shoulder surgery or infection
Activities and Risk Factors
Shoulder OA is commonly seen in individuals who have:
- A history of manual labour or repetitive overhead work (e.g., construction workers, plasterers, painters)
- Participated in overhead sports such as swimming, cricket, weightlifting, and tennis
- Had previous shoulder trauma or dislocations
- Family history of joint disease or osteoarthritis
Symptoms of Shoulder Osteoarthritis
Symptoms of shoulder OA typically develop gradually over time and worsen with activity. The onset may be subtle, starting with occasional discomfort and progressing to persistent pain and functional limitation.
Shoulder Pain
- Deep, dull aching pain in the shoulder, often centred around the back or top of the joint
- Pain may radiate to the upper arm or neck
- Worse with activity (especially overhead or behind-the-back movements) and after periods of rest
- Night pain is common and may affect sleep
Joint Stiffness
- Reduced range of motion, particularly for reaching overhead or rotating the arm
- “Freezing” or catching sensation as the joint stiffens
Grinding or Clicking
- Patients may feel or hear crepitus – a grating, grinding, or popping sound—due to roughened joint surfaces
Weakness and Loss of Function
- Difficulty performing routine tasks such as dressing, lifting a kettle, or driving
- Some patients compensate with abnormal movement patterns, leading to secondary neck or upper back pain
Diagnosis of Shoulder Osteoarthritis
Diagnosis of shoulder OA begins with a detailed clinical history and physical examination. Your specialist will assess:
- Pain location and pattern
- Range of motion (active and passive)
- Joint stability
- Strength and signs of rotator cuff involvement
Imaging
- X-rays: This is primary, gold standard diagnostic tool for OA. Common features include joint space narrowing, osteophyte formation, subchondral sclerosis, and bone cysts.
- MRI: Used to assess the integrity of the rotator cuff and detect early cartilage or soft tissue changes.
- Ultrasound: This may be used to assess surrounding structures such as bursae or tendons.
Differential Diagnosis
Other conditions can mimic shoulder OA symptoms and may coexist:
- Rotator cuff tear or tendinopathy
- Frozen shoulder (adhesive capsulitis)
- Impingement syndrome
- Cervical radiculopathy (nerve root compression)
- AC joint pathology independent of the glenohumeral joint
Treatment Options
Non-Surgical Management
The majority of patients with mild to moderate OA can manage their symptoms conservatively. These include:
- Physiotherapy: Tailored exercises to maintain range of motion, improve posture, and strengthen the surrounding musculature
- Activity modification: Avoiding repetitive overhead activity or heavy lifting where possible
- Pain relief: NSAIDs, paracetamol, and topical anti-inflammatories can be effective
- Corticosteroid injections: Offer temporary relief from inflammation and pain, particularly during flare-ups
- Hyaluronic acid injections (viscosupplementation): May be considered in early OA to improve lubrication
- Heat therapy, massage, and acupuncture as supportive measures
Surgical Treatment for Shoulder Osteoarthritis
Surgery is considered when conservative measures fail to provide adequate pain relief or when quality of life is significantly impacted.
Types of Surgery
Arthroscopic Debridement: Suitable for early-stage OA. Involves “cleaning out” the joint by removing loose cartilage, smoothing rough surfaces, and sometimes releasing tight joint capsules.
Hemiarthroplasty: Replaces only the humeral head (ball), used when the glenoid (socket) remains intact.
Total Shoulder Replacement (Anatomic TSR): Both the humeral head and glenoid are replaced with prosthetic components. Best suited for patients with intact rotator cuff function.
Reverse Shoulder Replacement: Used in cases where OA is combined with a large or irreparable rotator cuff tear (cuff tear arthropathy). The ball-and-socket orientation is reversed to rely on the deltoid muscle for shoulder movement.
Who Benefits from Surgery?
Surgery may be appropriate for:
- Patients with advanced OA who have exhausted non-surgical options
- Those with significant loss of function, sleep disturbance, or pain at rest
- Active individuals who wish to return to recreational or daily activities
- Patients with cuff tear arthropathy, where reverse shoulder replacement offers the best outcomes
Outcomes from Surgery
Shoulder replacement surgery has a high success rate, particularly when matched to the appropriate patient and OA severity. Most individuals experience:
- Significant pain reduction or resolution
- Improved range of motion and function
- Enhanced quality of life
Recovery time varies by procedure but generally involves 4-6 weeks of sling immobilisation and several months of physiotherapy. Long-term implant survival is excellent, especially in patients over 65.
FAQs
Can shoulder osteoarthritis be cured without surgery?
OA cannot be reversed, but many patients can manage their symptoms effectively with non-surgical options such as physiotherapy, medication, and lifestyle modifications.
How long do shoulder replacements last?
Modern shoulder prostheses can last 15–20 years or more, especially with proper post-operative care and avoiding excessive strain.
Will I regain full movement after shoulder replacement?
Most patients regain good functional range of motion. Full movement depends on the degree of pre-operative stiffness and whether the rotator cuff is intact.
Is there anything I can do to slow the progression of OA?
Maintaining good posture, performing regular shoulder-strengthening exercises, avoiding repetitive strain, and managing weight can help reduce the progression of OA.
How do I know if it’s OA or a rotator cuff tear?
Both conditions can cause pain and weakness, but OA is more associated with joint stiffness, grinding, and gradual onset. Imaging and clinical assessment help differentiate the two.