Acromioclavicular (AC) joint osteoarthritis is a common cause of shoulder pain, particularly in middle-aged and older adults. It involves the gradual wear and tear of the cartilage in the small joint where the collarbone (clavicle) meets the highest point of the shoulder blade (acromion). This degeneration can lead to pain, stiffness, and reduced function in the shoulder, particularly during overhead or cross-body movements. In many people, AC joint osteoarthritis develops as a result of ageing, past injury, or repetitive strain from sports or manual work.
Anatomy of the AC Joint
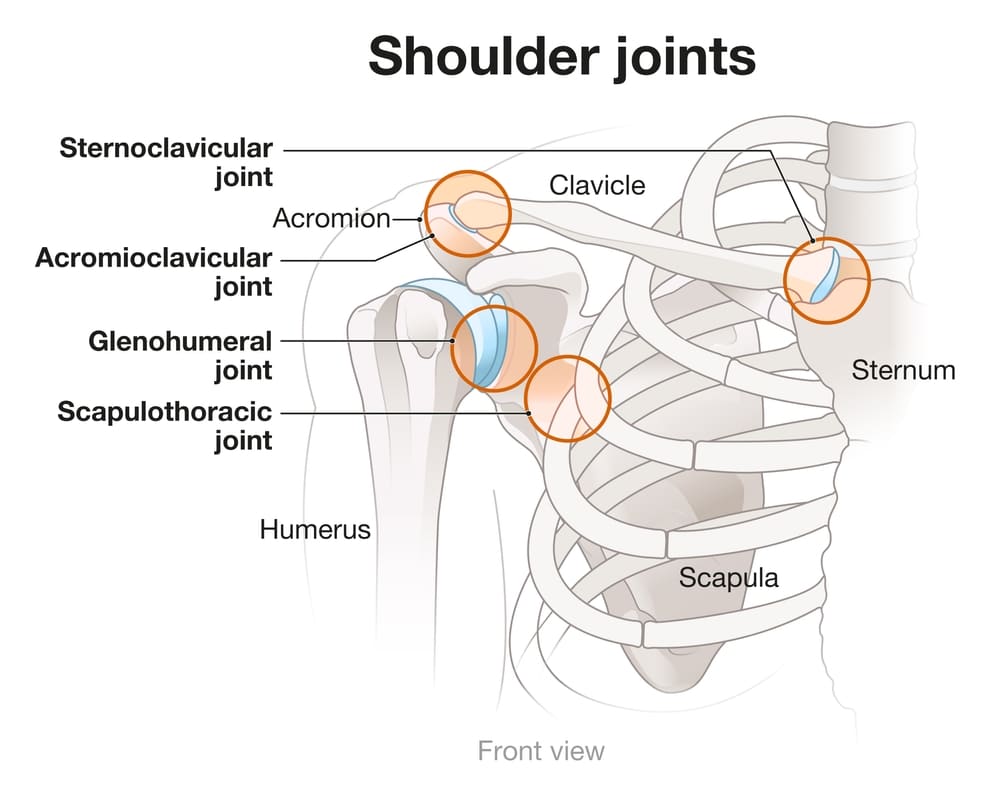
The AC joint is located at the top of the shoulder, where the clavicle (collarbone) meets the acromion, part of the scapula (shoulder blade). It is a small but vital joint that allows fine-tuned movement of the shoulder, especially when raising the arm or moving it across the body. The joint is lined with cartilage and contains a disc for cushioning, which helps the bones glide smoothly against one another. Ligaments surrounding the joint help stabilise it.
Over time or due to injury, the cartilage may wear down, causing the bones to rub directly against each other—leading to osteoarthritis.
Causes of AC Joint Arthritis
AC joint osteoarthritis often develops gradually due to cumulative wear and tear, but may also be post-traumatic. The condition arises when the cartilage that cushions the joint surfaces wears down, causing the clavicle and acromion to rub together painfully.
Key causes and risk factors include:
- Age-related degeneration: Over time, repetitive micro-movements and weight bearing through the joint cause cartilage thinning and eventual degradation.
- Previous AC joint trauma: Past injuries such as a shoulder separation (AC joint sprain) or clavicle fracture can alter the joint mechanics, leading to earlier onset OA.
- Postural and biomechanical stress: Shoulder girdle imbalances, poor thoracic posture, or scapular dyskinesis can result in abnormal joint loading and degenerative changes over time.
- Genetics and systemic conditions: While less common, certain individuals may have a genetic predisposition to earlier or more severe OA. Additionally, conditions like rheumatoid arthritis can hasten joint degeneration.
- Repetitive overhead or cross-body activities: These movements load the AC joint and accelerate cartilage wear.
Commonly affected individuals include:
- Weightlifters (especially with heavy bench pressing or shoulder presses)
- Swimmers and rowers
- Tennis and racket sport players (from repetitive arm movement and stress on the shoulder girdle)
- Manual labourers (e.g., carpenters, plasterers, electricians)
- CrossFit enthusiasts and athletes involved in overhead lifting or gymnastics-based routines
Symptoms of AC Joint Arthritis
Symptoms may develop gradually over months or years, or acutely following an injury or flare-up of a previously quiet joint.
Common symptoms include:
Localised pain on top of the shoulder: Patients typically point directly to the AC joint. Pain is often dull or achy at rest, becoming sharp or catching with movement.
Pain during specific arm movements:
- Overhead activities (e.g. lifting weights, reaching for shelves)
- Cross-body actions (e.g. putting on a seatbelt, hugging)
- These movements compress the joint, causing discomfort.
Swelling and bony prominence: Chronic AC joint OA can lead to hypertrophy of bone and visible joint thickening or a palpable lump.
Clicking or crepitus: As the cartilage wears away, the joint surfaces grind, producing audible or palpable creaking.
Night pain: Discomfort is often worse when lying on the affected side or due to cumulative inflammation from daily activity.
Loss of shoulder range and strength: In longstanding cases, patients may unconsciously avoid certain positions, leading to reduced motion or muscle deconditioning.
How Do We Diagnose AC Joint Arthritis?
A thorough subjective and clinical assessment is essential.
Diagnosis typically includes:
History and physical examination: The clinician will examine the location of pain and use specific tests such as the cross-body adduction test, where the patient moves the arm across the chest to elicit AC joint pain.
Imaging
- X-ray: Often shows joint space narrowing, osteophyte (bone spur) formation, and sclerosis of the bone ends.
- Ultrasound or MRI: May be used if other shoulder pathologies are suspected or to assess inflammation and surrounding soft tissues.
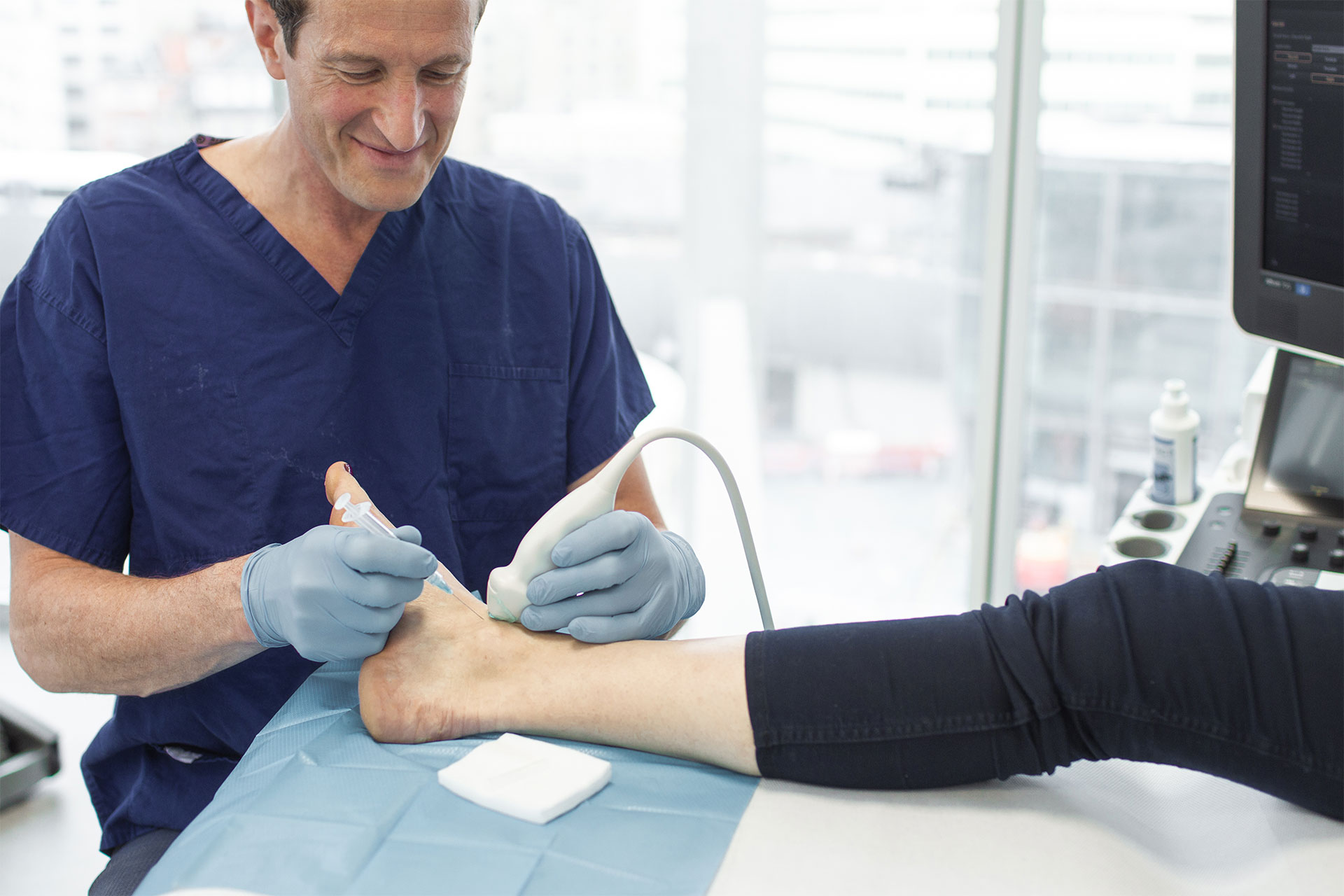
- Diagnostic injection: A targeted local anaesthetic injection into the AC joint can confirm the diagnosis if it temporarily relieves pain.
Differential Diagnosis
Several other conditions can mimic or occur alongside AC joint OA:
- Rotator cuff tendinopathy or tear
- Shoulder impingement syndrome
- Glenohumeral joint osteoarthritis
- Frozen shoulder (adhesive capsulitis)
- Distal clavicle osteolysis (in younger athletes or weightlifters)
- Post-traumatic AC joint separation
A careful clinical examination and imaging help consolidate findings and ensures an accurate diagnosis.
Treatment Options For AC Joint Arthritis
Non-Surgical Management
Most patients can manage AC joint OA with conservative approaches:
- Activity modification: Avoiding aggravating movements such as heavy lifting or overhead work.
- Physiotherapy: To strengthen shoulder stabilisers, correct postural imbalances, and maintain range of motion.
- Anti-inflammatory medications: NSAIDs (e.g. ibuprofen) can reduce pain and inflammation.
- Ice therapy: Applying ice over the joint after activity can reduce swelling and discomfort.
- Corticosteroid injection: Ultrasound-guided injection into the AC joint can provide temporary relief, especially during flare-ups or in early to moderate disease.
Surgical Options
Surgery is considered when pain persists despite non-operative treatment or when symptoms significantly affect daily life or athletic performance.
The most common procedure is an arthroscopic distal clavicle excision, also known as the Mumford procedure. This involves removing a small portion of the clavicle to prevent painful contact between the bones.
Key benefits:
- Performed using minimally invasive (keyhole) techniques
- Preserves the surrounding ligaments and muscle attachments
- Usually a day-case procedure with rapid recovery
Who benefits from surgery:
- Active individuals or athletes with ongoing pain despite conservative treatment
- Those with mechanical symptoms such as catching or grinding
- Patients with advanced joint degeneration seen on imaging
Outcomes of AC Joint Surgery
Surgical outcomes are generally excellent, with high rates of pain relief and return to function. Most patients regain full shoulder motion and resume sports or manual work within 2–3 months post-operatively, following a brief course of physiotherapy.
Frequently Asked Questions
Can AC joint arthritis heal on its own?
No, osteoarthritis is a degenerative condition. While symptoms can be managed and flare-ups reduced, the underlying joint damage does not reverse.
How is AC joint arthritis different from other shoulder arthritis?
AC joint OA affects the small joint at the top of the shoulder, whereas glenohumeral OA involves the main ball-and-socket shoulder joint. Pain in AC joint OA is typically more localised and linked to specific movements.
Is surgery always needed?
Not at all. Many patients manage well with conservative measures like physiotherapy and injections. Surgery is reserved for persistent or severe cases.
What activities should I avoid with AC joint arthritis?
Limit heavy lifting, overhead work, and movements that bring the arm across the body. Modifying your gym routine and correcting posture may also help.
How long does it take to recover from AC joint surgery?
Recovery is usually straightforward. Most patients return to light activity within 2–3 weeks and resume sports or manual work within 2–3 months.