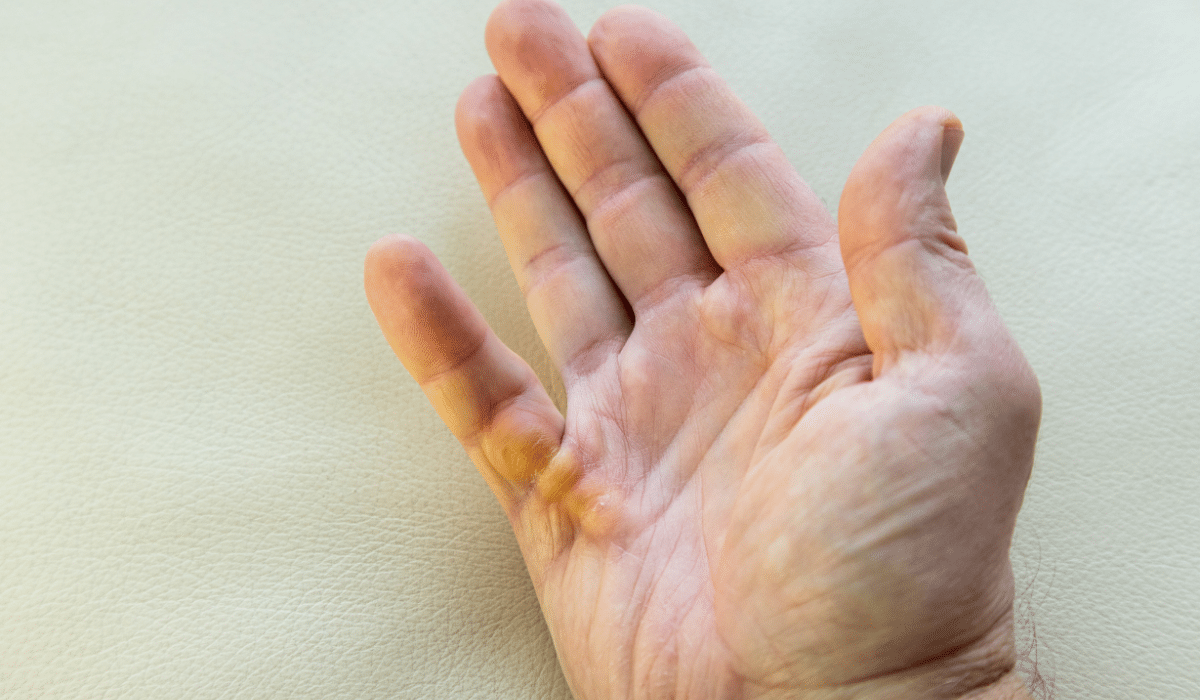
Dupuytren’s disease, also known as Dupuytren’s contracture, is a progressive condition that affects the connective tissue in the palm of the hand. This disorder leads to the formation of thickened, scar-like tissue beneath the skin, causing the fingers to bend inward towards the palm, resulting in difficulty straightening them. While Dupuytren’s disease primarily affects the hands, it can also occur in other parts of the body, such as the feet.
At London Bridge Orthopaedics we have three expert hand specialists who regularly treat this condition.
In this blog, we will explore the anatomy, causes, symptoms and management options for Dupuytren’s disease and contracture.
Anatomy of the Hand
To understand Dupuytren’s disease, it is essential to first grasp the anatomy of the hand. The hand is a complex structure composed of bones, muscles, tendons, ligaments, and connective tissue, all working together to facilitate movement and dexterity. The palm of the hand contains a dense network of fibrous tissue called the palmar fascia, which provides support and stability to the hand and fingers. In individuals with Dupuytren’s disease, this palmar fascia becomes thickened and contracted, leading to the characteristic bending of the fingers.
Causes of Dupuytren’s Disease
It is unclear what the exact cause of Dupuytren’s disease is, but several risk factors have been identified, including:
- Genetics: Dupuytren’s disease often runs in families, suggesting a genetic predisposition to the condition. Certain gene mutations may increase the likelihood of developing abnormal fibrous tissue in the hands.
- Age: Dupuytren’s disease is more common in older adults, with the risk of developing the condition increasing with age.
- Gender: Men are more likely than women to develop Dupuytren’s disease, particularly after the age of 40.
- Ethnicity: Individuals of Northern European descent, particularly those of Scandinavian or Celtic ancestry, have a higher incidence of Dupuytren’s disease.
- Lifestyle Factors: Smoking, alcohol consumption, and manual labour have been associated with an increased risk of developing Dupuytren’s disease, although the exact mechanisms are not fully understood.
Mechanism of Injury
The underlying mechanism of injury in Dupuytren’s disease involves the abnormal proliferation of fibroblasts, specialised cells responsible for producing collagen and other components of connective tissue.
In individuals with Dupuytren’s disease, these fibroblasts become overactive, leading to the excessive production of collagen and the formation of fibrous nodules and cords within the palmar fascia. As these cords contract and tighten over time, they pull the affected fingers into a flexed or bent position, resulting in the characteristic contracture seen in Dupuytren’s disease.
Symptoms of Dupuytren’s Disease
Many of the symptoms of Dupuytren’s disease typically develop gradually and may include:
- Thickening and puckering of the skin on the palm of the hand, particularly near the base of the fingers.
- Formation of small, tender nodules or lumps beneath the skin.
- Progressive tightening and bending of one or more fingers, usually the ring finger and little finger.
- Difficulty straightening the affected fingers or fully extending them.
- Diminished grip strength and dexterity, making it challenging to perform everyday tasks such as grasping objects or shaking hands.
Diagnosis of Dupuytren’s Disease
Diagnosing Dupuytren’s disease is usually based on a combination of understanding a patient’s medical history, a thorough physical examination of the hands, and imaging studies. During the physical examination, your consultant will assess the degree of finger contracture, palpate for nodules or cords in the palm, and evaluate the patient’s range of motion.
Imaging modalities such as ultrasound or magnetic resonance imaging (MRI) may be used to visualise the extent of fibrous tissue involvement and assess the severity of the condition.
Nonsurgical Management of Dupuytren’s Disease
While there is no cure for Dupuytren’s disease, nonsurgical management options may help alleviate symptoms and slow the progression of contracture.
Non-surgical options for Dupuytren’s contracture may include
- Observation: In mild cases of Dupuytren’s disease with minimal symptoms, observation may be recommended to monitor disease progression without intervention.
- Physical Therapy: Performing stretching exercises, massage, and hand therapy techniques to improve finger flexibility, strengthen the hand muscles, and maintain range of motion.
- Splinting: Wearing a custom-made splint or orthosis to support the affected fingers and prevent further contracture.
- Enzyme Injections: Injecting collagenase enzyme (Xiaflex) into the fibrous cords to weaken and break down the scar tissue, allowing for manual manipulation and straightening of the affected fingers.
Surgical Management of Dupuytren’s Disease
In advanced cases of Dupuytren’s contracture where nonsurgical treatments are ineffective or the contracture is severe, surgical intervention may be necessary to release the tight bands of tissue and restore finger mobility.
Surgical options for Dupuytren’s Disease contracture may include
- Fasciotomy: Making small incisions in the palm or finger to release the contracted bands of tissue and improve finger extension.
- Fasciectomy: Removing the diseased portion of the palmar fascia through open or minimally invasive surgery to eliminate the source of contracture.
- Needle Aponeurotomy: Inserting a needle into the fibrous cords under local anesthesia and manually breaking them apart to release tension and straighten the affected fingers.
- Dermofasciectomy: Excising both the affected palmar fascia and overlying skin to address severe contracture and prevent recurrence.
Conclusion
Dupuytren’s disease and contracture can significantly impact hand function and quality of life for affected individuals.
If you are suffering for any of the symptoms described above or have an issue with your hand or wrist please get in touch with us to book an appointment with one of our Hand and Wrist Consultants.
You can book an appointment with any of our Hand and Wrist consultants by calling our booking team or filling out an online appointment request today